Yeast like germs found in facial seborrhea (Malassezia and Candida species), and other fungi have been found in brains of alzheimer victims. Prior untreated facial cold sores increase dementia rate 3-10 fold. The beta amyloid we were so worried about is toxic to these organism and now thought to be just a protective agent. Mouse model of alzheimer’s is now shown to get candida granulomas in the brain. Very quickly there may be a paradigm shift of thinking of alzheimer causes from brain crud problem to infection. Researchers have also found an agent to interfere with prion virus like particles found in dementia. And now, more recently, gum disease bacteria is thought to be a major player in both dementia and maybe coronary artery disease. New theory links clotting factor leakage in brain to dementia.
This topic is difficult because it is evolving so quickly but I will try to be as clear as I can.
They have used various technique to remove Beta amyloid without any benefits. Recently they found that beta amyloid is good at fighting infection so there has been a shift in feeling about it.
The Cold Sore Connection
Tzeng, Nian-Sheng, et al.
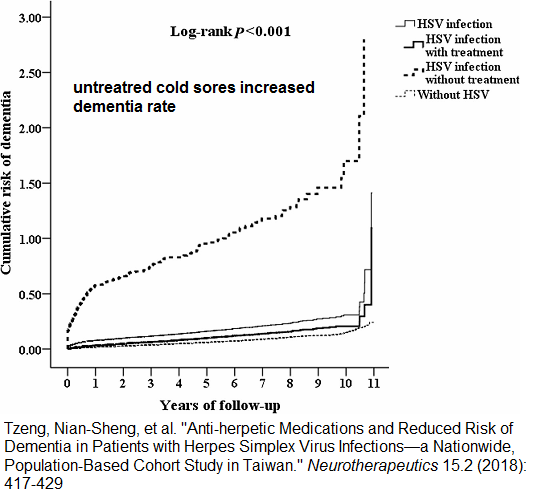
Anti-herpetic Medications and Reduced Risk of Dementia in Patients with Herpes Simplex Virus Infections—a Nationwide, Population-Based Cohort Study in Taiwan. Neurotherapeutics 15.2 (2018): 417-429
https://link.springer.com/article/10.1007/s13311-018-0611-x
- People who have UNTREATED cold sore in later years end up with 3-10 times the alzheimer rate.
- I had one lady that I treated well until her 90’s without significant mental deterioration. Then she had a bad cold sore outbreak and came in too late for treatment to offer much. Subsequently, she has quickly deteriorated though she is on valcyclovir prophylaxis now.
- here is an accumulative graph showing run away dementia in untreated cold sore victims ( versus those treated showing no increase):
There is a chronic pain connection related to APO-E4 – a lipid protein:
- It is well known that APO E4 noted for increasing risk of head injury damage and dementia. Add in poor sleep from insomnia and more common then recognized sleep apnea with APO E4, the dementia risk much worse:
Int Psychogeriatr. 2016 Sep;28(9):1409-24. doi: 10.1017/S1041610216000405
Associations between depression, sleep disturbance, and apolipoprotein E in the
development of Alzheimer’s disease: dementia.
Burke SL et al
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4963299/ - Having the APO E4 gene makes post-traumatic fibromyalgia at least 3.7 times more likely (relative risk 7.06 versus 1.9 in controls)
Reeser, Jonathan C., et al.
Apolipoprotein e4 genotype increases the risk of being diagnosed with posttraumatic fibromyalgia.
PM&R 3.3 (2011): 193-197.
https://www.sciencedirect.com/science/article/pii/S1934148210013584 - APO E4 positivity increased herpetic lesion rates 4.6 fold
Sex Transm Infect. 2010 Jun;86(3):202-6.
APOE genotype is associated with oral herpetic lesions but not genital or oral herpes simplex virus shedding.
Koelle DM et al
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2881187/ - Older (50+) and get cold sore lesions? – at least have valcylovir to take 2 gm x2 doses q12 h when outbreak and consider 500 mg daily prophylaxis. Lip gloss with paba in it would be good against sun exposed outbreaks
- Facial shingles/zoster will triple your dementia rate so for Gd’s sake get zoster vaccinated
Fungal Connection:
- Many years back I can remember infection element being noted in brains of dementia victims but being dismissed as artifacts
- 2014 things changed with more modern techniques highlighting fungal element – though not many
J Alzheimers Dis. 2014;41(1):301-11. doi: 10.3233/JAD-132681.
Fungal infection in patients with Alzheimer’s disease.
Alonso R et al
https://content.iospress.com/articles/journal-of-alzheimers-disease/jad132681 - this has been recently confirmed in a 2018 study:
Front Aging Neurosci. 2018 May 24;10:159. doi: 10.3389/fnagi.2018.00159
Infection of Fungi and Bacteria in Brain Tissue From Elderly Persons and Patients
With Alzheimer’s Disease.
Alonso R et al.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5976758/
“the fungal genera more prevalent in AD patients were Alternaria, Botrytis, Candida, and Malassezia” - Introducing a mild candida IV infection in mice will trigger Alzheimer like state in the brains:
Microglia and amyloid precursor protein coordinate control of transient Candida cerebritis with memory deficits
Yifan Wu, Shuqi Du, Jennifer L. Johnson, Hui-Ying Tung, Cameron T. Landers, Yuwei Liu, Brittany G. Seman, Robert T. Wheeler, Mauro Costa-Mattioli, Farrah Kheradmand, Hui Zheng & David B. Corry
nature communications 10(1) January 2019
https://www.nature.com/articles/s41467-018-07991-4 - good discussion of this new article here:
Mouse Memory Affected by Mild Fungal Infections
https://www.genengnews.com/news/mouse-memory-affected-by-mild-fungal-infection/ - Now recall that two fungal elements included Candida ( yeast) and Malassezia – both know for their propensity to be on the skin of subjects with seborrhiec dermatis and also found in dandruff
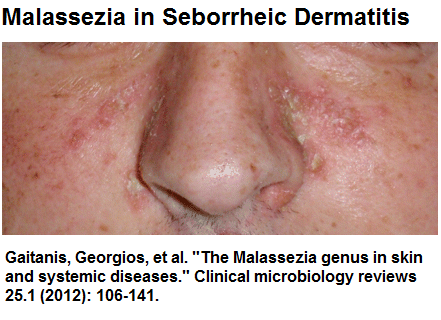 topical agents and shampoos – selsun blue and nizoral can help but I feel as systemic drug is needed:
topical agents and shampoos – selsun blue and nizoral can help but I feel as systemic drug is needed:
Zisova, Lilija G.
Fluconazole and its place in the treatment of seborrheic dermatitis–new therapeutic possibilities.
Folia medica 48.1 (2006): 39-45.
https://europepmc.org/abstract/med/16918053
fluconazole 50 mg/day x2wks only -“In 74% of the patients the specific test for Malassezia spp. was negative after treatment”
I think it would be wise to take 50 mg bid for 2 weeks…just a 300 mg dose once weekly does not cut it:
Cömert, Asuman, et al.
Efficacy of oral fluconazole in the treatment of seborrheic dermatitis.
American journal of clinical dermatology 8.4 (2007): 235-238.
https://link.springer.com/article/10.2165/00128071-200708040-00005
“marginal benefit”Comment – So some things are obvious but you need to start with basics - see a doctor – make sure blood pressure and diabetes issues are well attended to
- Don’t smoke
- Aerobic exercise most days of the week ( I get up at 7 am to go – still waiting to enjoy it)
- Get enough sleep and make sure you do not have sleep apnea if positive – use CPAP – not just a mouth guardBased on above literature I would:
1) get a shingles vaccine2) get any cold sore outbreaks treated and consider Valtrex prolylaxis and PABA sunscreen lip gloss3) I have seborrhea and I’m going to take flucanazole 50 mg bid x2 weeks every 3 months in my post 65 age state..
Prion Disease
- addendum – what was not mentioned was the prion like infection found in dementia victims. Now, researchers have found an agent that could bind to prion particles and rescue mice affected with Creutzfeldt-Jakob Disease
Gunther, Erik C., et al.
Rescue of Transgenic Alzheimer’s Pathophysiology by Polymeric Cellular Prion Protein Antagonists.
Cell Reports 26.1 (2019): 145-158.
https://www.cell.com/cell-reports/fulltext/S2211-1247(18)31932-6
Good writeup from Yale on it here:
New compound shows promise in treatment of Alzheimer’s
https://news.yale.edu/2019/01/02/new-compound-shows-promise-treatment-alzheimers
Gum Germ Disease
Porphyromonas gingivalis in Alzheimer’s disease brains: Evidence for disease causation and treatment with small-molecule inhibitors
Stephen S. Dominy et al
Science Advances 23 Jan 2019:
Vol. 5, no. 1, eaau3333
DOI: 10.1126/sciadv.aau3333
http://advances.sciencemag.org/content/5/1/eaau3333
- transgenic mice overexpressing mutated human amyloid precursor protein (hAPP-J20), oral infection with P. gingivalis impairs cognitive function, increases the deposition of AD-like plaques, and results in alveolar bone loss compared to control hAPP-J20 mice (15).
- P. gingivalis lipopolysaccharide has been detected in human AD brains (16), promoting the hypothesis that P. gingivalis infection of the brain plays a role in AD pathogenesis
- P. gingivalis secretes a toxin called gingipain which are found by antibody tagging in brains of Alzheimer victims

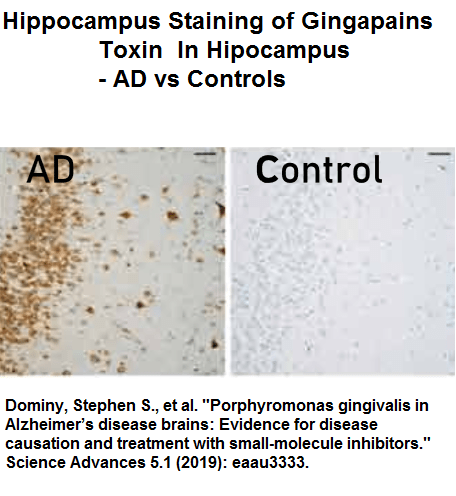
But this is just the tip of the iceburg:
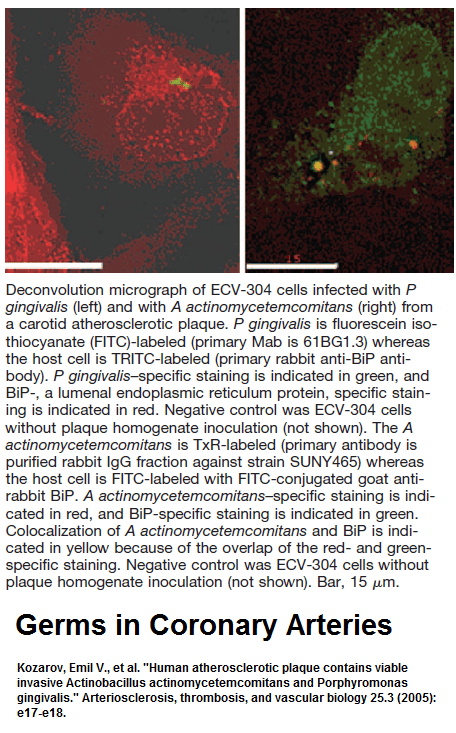
gingival germs are found in samples of coronary arteries during bypass procedure:
Porphyromonas gingivalis is the most abundant species detected in coronary and femoral arteries.
Journal of oral microbiology 9.1 (2017): 1281562.
https://www.tandfonline.com/doi/abs/10.1080/20002297.2017.1281562
Kozarov, Emil V., et al.
Human atherosclerotic plaque contains viable invasive Actinobacillus actinomycetemcomitans and Porphyromonas gingivalis.
Arteriosclerosis, thrombosis, and vascular biology 25.3 (2005): e17-e18.
https://www.ahajournals.org/doi/full/10.1161/01.atv.0000155018.67835.1a
https://newpainmuse.org/2018/12/31/cognitively-impaired-elderly-have-high-likelihood-of-dental-issues-and-orofacial-pain/
Comment :
Addendum:
an alternate theory of dementia has just been released linking extravasation of fibrinogen into tissues to activation of glial cells which leads to brain inflammation:
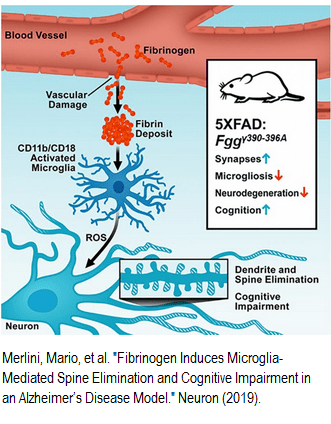
Merlini, Mario, et al.
Fibrinogen Induces Microglia-Mediated Spine Elimination and Cognitive Impairment in an Alzheimer’s Disease Model.” Neuron (2019) in press
https://www.sciencedirect.com/science/article/pii/S0896627319300157
discussed here:
https://www.genengnews.com/news/alzheimers-cognitive-dysfunction-linked-to-clotting-factor/
Addendum – field of dementia is changing so fast. Study found that consumption of mushrooms twice weekly could reduce early dementia (mild cognitive impairment) by 50%:
The Association between Mushroom Consumption and Mild Cognitive Impairment: A Community-Based Cross-Sectional Study in Singapore
Feng, Leia et al
Journal of Alzheimer’s Disease, vol. 68, no. 1, pp. 197-203, 2019
https://content.iospress.com/articles/journal-of-alzheimers-disease/jad180959
a news release about it here:
http://news.nus.edu.sg/research/mushrooms-reduce-cognitive-decline
–